Happy New Year! It’s has been a great start to 2016 for our Medical Capacity Building team here in Madagascar. We have now introduced the WHO Surgical Safety Checklist at 16 hospitals across the country, so we were very excited to start re-visiting some of these teams 3-4 months on for follow up, alongside continuing to run courses.
We approached our first follow up visits with a mixture of excitement and trepidation. George Bernard Shaw famously commented that the single biggest problem in communication is the illusion it has taken place! It’s no small thing to ask for a change in daily practice from an entire team, using a Checklist together during surgery is a completely unfamiliar process to most of those we have trained. We hoped that the new Lifebox pulse oximeters we donated would be used routinely not only during surgery, but in the recovery areas after surgery too. What’s more, just before Christmas one of the courses required us to communicate in English, French, Malagasy and Chinese! Would the teams still be doing the Checklist 3-4 months on? Will the Lifeboxes be helping? We were not sure what we would find…
“Every act of communication is an act of tremendous courage in which we give ourselves over to two parallel possibilities: the possibility of planting into another mind a seed sprouted in ours and watching it blossom into a breathtaking flower of mutual understanding; and the possibility of being wholly misunderstood.” Maria Popova
Following up:
We kicked off with visiting our friends in Sambava and Antalaha, two of the first hospitals to implement the Checklist in October last year. Thanks to the Lifebox pulse oximeter donations, Antalaha have been able to safely open a second operating room, and are now able to help many more patients. On this follow-up visit we also were able to supply them with equipment to monitor blood pressure and some child-sized anesthesia equipment to continue to improve the safety of the surgeries offered.
In Sambava their main challenge came from the fact that many of their theatre team were Chinese, and didn’t speak French or Malagasy! At the follow up we were able to work with a Chinese doctor who spoke French. Using the WHO materials published in Chinese, we added a Chinese translation alongside the Sambava team’s French locally adapted checklist so that the whole team can now do the checks together!
Both teams also reported better communication and atmosphere in theatre with inclusion of the whole team, and increased confidence in the safety of their processes. Both also told stories of how the checklist had helped them to avoid making serious errors, such as patients getting mixed up in emergencies and the wrong patient getting the wrong surgery.

Translating the adapted checklist into Chinese. We also worked with the Opthalmologist (far right) to develop a specifically adapted checklist for use in the eye operating room.
Lifeboxes: Truly boxes that save lives!
During follow up phone calls this week we heard stories from two different hospitals about very unwell patients who made it through major surgery, but had suddenly and unexpectedly deteriorated after their operations. Both teams reported that at the time, there was no other obvious warning that things had changed, it was the alarm from the Lifeboxes which alerted them to the sudden life-threatening plummeting oxygen levels, this gave the team the vital seconds they needed to react and resuscitate these patients in time to save their lives. These stories are so encouraging, as my manager Krissy Close said ‘lives have already been protected and operating room teams transformed. Nurses feel empowered, surgeons feel protected, and patients are better cared for… this is what it’s all about!’
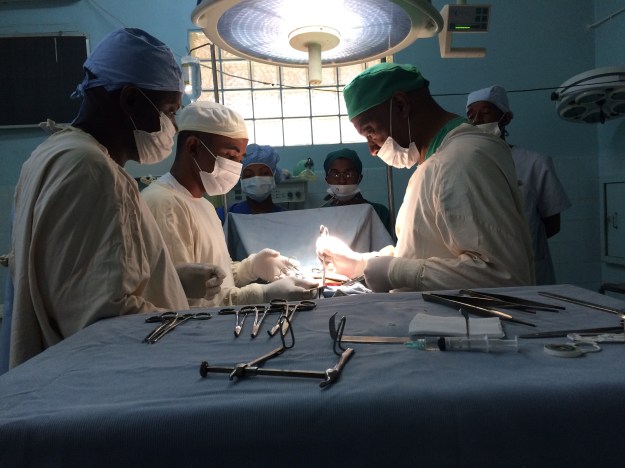
Checklist, Lifeboxes, and surgical instruments and swab counting put into practice in theatre
Courses continue
Back in teaching mode, our team of 3 continued on to Manakara where we held the largest teaching session so far, 28 people! We had fantastic support from the regional Minister of Health, who attended both the opening and closing ceremonies, and the hospital personnel were very enthusiastic. Farafangana also were very receptive, and during the course we were able to join the team in theatre for 3 real cases. This has proved hugely beneficial, as we have seen the Checklist being confidently used and the Lifeboxes introduced into the theatre and recovery before we leave the hospital. It has also been fascinating for me to spend time teaching and discussing in theatre with the nurse anaesthetists, (there are very few doctor anaesthetists here) who do an incredible job with great flexibility and resourcefulness in situations where materials, medications and equipment can be hard to come by. For example, Ketamine is a medication which has recently narrowly escaped changes to international regulations that would affect it’s availability. At home people may have heard of Ketamine as a drug of abuse, but in most hospitals here, it is an essential part of anaesthesia provision. See the World Federation of Societies of Anesthesiologists (WFSA) ‘Ketamine is medicine’ campaign for more.
Tomorrow at mid day we head off for 2 weeks of follow up visits, during which we will re-visit 5 different hospital teams around the country, and later in February Checklist courses will continue. I’m sure we will have more stories to tell!

Some of the team from Farafangana with Dr Nandi and Dr Hasina

Well done Linden for all that you and the team are doing. Blessings to you all xx
LikeLike